Looking after and maintaining dental implants
Just like natural teeth in the mouth, dental implants have a gum (also called mucosal) layer around the top part. The implant tops and new teeth above them need daily cleaning and flossing to protect the gum (mucosa) and the bone attachment.
It is possible to develop inflammation around implants in the same way that gum disease can develop around teeth. The cause of this can include poor cleaning, smoking, genetic predisposition, ill-fitting crowns and/or excess dental cement under the crowns. The name of this inflammation is peri-implant mucositis which might be thought of as an early warning. If untreated, a more serious problem called peri-implantitis can develop which is better defined as an infection of the bone supporting the implant.
Peri-implant Mucositis
As discussed above, this condition may be the first sign that the gum or mucosa around the implant is not in perfect health. Inflammation may be present, with bleeding and pocket formation, and the mucosal attachment to the titanium abutment may have become weakened. Typically, when probing around the implant there will be spontaneous bleeding and the mucosa may be tender. The gum is more red/mauve and less pink in colour. However the bone underneath is unaffected and there is no evidence of pus or an infection.
The condition is better treated conservatively with antimicrobial solutions and topical antibiotics. Advice on different ways to clean the area may be needed and alternative technology supplied to produce better levels of oral hygiene. Any possible causes for the inflammation such as excess dental cement may need to be addressed to prevent recurrence. In any event, close monitoring and repeat therapy may be indicated occasionally.
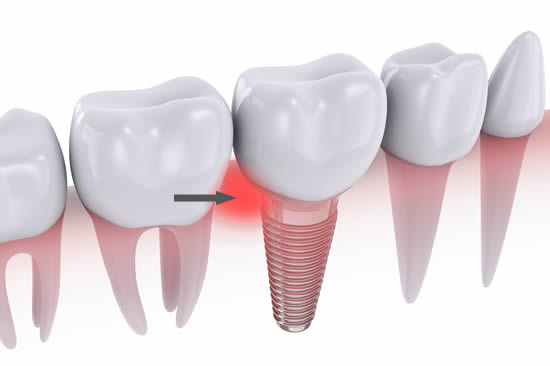
Peri-implantitis
Peri-implantitis is quite similar to periodontal (gum) disease around the teeth. There will be mucositis (see above; peri-implant mucositis) but with underlying infection (pus) and a loss of bone around the implant itself. An X-ray will confirm this. Other relevant factors are smoking, poor oral hygiene and systemic conditions such as diabetes.
The treatment for peri-implantitis is initially similar to that for peri-implant mucositis, i.e. irrigation under the gum with antimicrobial agents but also with the topical application of antibiotic gels below the gum and into the pockets that form deeper down into the bone.
If the more conservative treatment fails to remove the infection or if the disease has progressed too far then surgical decontamination is required. This involves raising the gum, just as at the implant placement stage, to remove the inflamed and infected tissue from around the implant(s) and to decontaminate the surface of the implant(s) which may be compromised. It might be necessary to undertake some form of bone grafting to repair any resultant defects. Local anaesthetic is usually fine, just as with implant placement, but sometimes sedation might be used at the same time.
In cases where the bone loss around the implants renders the area impossible to stabilise then the implants will need to be removed. We can often repair the damage and subsequently replace the implant(s), thus restoring you to full dental health. You would then remain on regular recalls to ensure that the disease is kept at bay and does not affect your new implant(s).

Fracture of Crowns, Bridges, or Dentures on Implants
Just as it is possible to break crowns or bridges on teeth, and teeth themselves, it can be possible to fracture the new “Teeth” on top of the implants. This complication can usually be overcome by sending the prosthetic teeth back to the laboratory where either a remake or a repair can be carried out. Occasionally, when the implant teeth have been functioning for a longer period of time, new crowns or bridges or dentures will need to be made.
